Introduction | Symptoms | Diagnosis | Treatment
Introduction
An abscessed tooth is an infected tooth. Your teeth contain tiny canals called root canals. Your root canals and the interior of your teeth contain pulp. Pulp is commonly infected by an untreated cavity. An untreated cavity can lead to a “pus-pocket” or abscess. Abscessed teeth are treated with root canal therapy. If left untreated, an abscessed tooth will eventually need to be removed.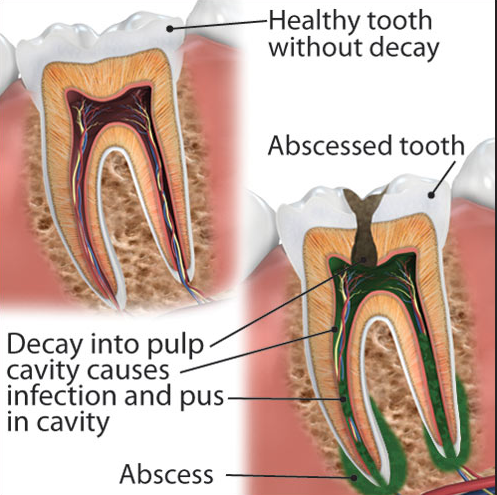
Pulp contains blood vessels, nerves, and connective tissue. Pulp nourishes teeth when they first emerge and are forming. When a tooth is mature, it is supported by a blood supply that establishes around the tooth.
Pulp can be infected as a result of damage, trauma, and tooth decay. A cavity can extend through the layers of a tooth. Tooth decay can lead to infection if it extends through the tooth’s outer layers (the enamel and dentin) and into the pulp and root canal. The opening created by a cavity allows bacteria to access and infect the pulp.
A pulp infection needs to be treated with root canal therapy. If a pulp infection is not treated, your tooth may need to be removed, and your infection may spread. A pulp infection can form an abscess and spread to your gum and jawbone. From there, it may spread to other parts of your body, including your brain, and cause serious medical conditions.
Symptoms
A pulp infection or abscess may not cause symptoms at first. You may notice symptoms in a tooth that has broken, cracked, or changed color. As a pulp infection progresses, you may experience pain and swelling around the affected tooth. Your tooth pain may increase dramatically when you bite down, touch, or put pressure on the tooth. Your tooth may be very sensitive to hot or cold temperatures. This may cause abrupt discomfort when you eat or drink hot or cold foods and beverages.Diagnosis
Your dentist can determine if you have an abscessed tooth by performing a dental examination. Your dentist may take X-rays to view the inside structure of your tooth. To test the sensitivity of your tooth, your dentist will gently tap your tooth and place hot and cold temperatures on it. Additionally, your dentist will inspect your gums for swelling.Your dentist may conduct further tests to help identify and determine the extent of a pulp infection. An electrical pulp tester is used to find out if the pulp is alive. The device sends a small electrical current through the tooth. You may feel a temporary tingling sensation while the test is conducted. The test does not cause pain or electrical shock.
Treatment
A dentist or an endodontist can perform root canal therapy. An endodontist is a dentist that specializes in diseases of the pulp and its surrounding tissues. Root canal therapy can require one or more visits to your dentist, depending on your tooth’s condition. An abscessed tooth may require more visits.Your dentist will numb your gums surrounding the affected tooth so that you will not feel any pain during the procedure. You may be sedated as well. Your dentist will use a very fine drill to create a small hole in the top or back of the tooth to access the pulp. Your dentist will remove the infected pulp.
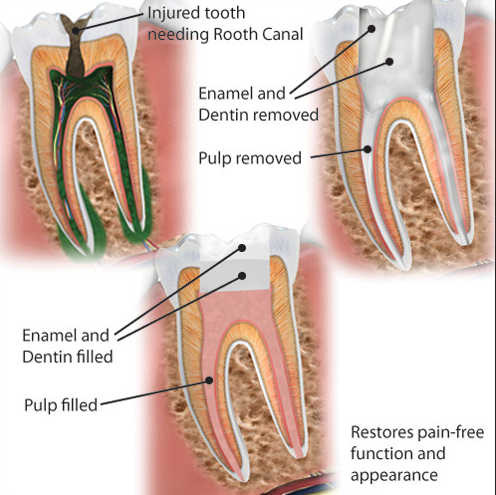
Your dentist will measure the size of the tooth’s root canals. Your dentist may use X-rays and an apex locator to measure their lengths. An apex locator uses a small harmless electrical current to calculate the length of the canal. Your dentist needs to know the length of the root canals for treatment planning.
After the root canals are measured, they are cleaned with special instruments. All of the canals in the tooth need to be cleaned. They are shaped to receive fillings and an antiseptic solution is applied to treat the infection. Next, the root canals are filled with an elastic material and anti-infection medication. The tooth will receive a temporary filling between dental visits or the tooth may be left open to help it heal. You may receive medication at this time for the infection. The tooth is permanently sealed with a crown.
Root canal therapy relieves the symptoms of infected pulp. Your restored tooth has the potential to remain healthy for a very long time. Practice good oral health care and receive regular dental check ups to ensure the integrity of your teeth.
This information is intended for educational and informational purposes only. It should not be used in place of an individual consultation or examination or replace the advice of your health care professional and should not be relied upon to determine diagnosis or course of treatment.



